Tough Calls: Case 6
Large Coronary Fistula
Imagine how you would work through each case. What equipment would you select and what would you do first? After having a go at it, see what our panel would do in the same situation. This exercise highlights the many possible approaches to a difficult problem. By seeing what others would do after thinking it through yourself, you will gain an understanding of the spectrum of approaches to a problem.
History
- 28 year old lady
- Symptoms: increasing shortness of breath, occasional palpitations, denies chest pain
- No indications of ischemia. No infections. No enlargement of right ventricle.
- Coronary angiogram showed large fistula circumflex to coronary sinus with OM branches coming off the fistula
- QP/QS: 1.93:1 on cardiac catheterization
Would you close this fistula? If so, how and why?
Should there be therapy post-procedure?
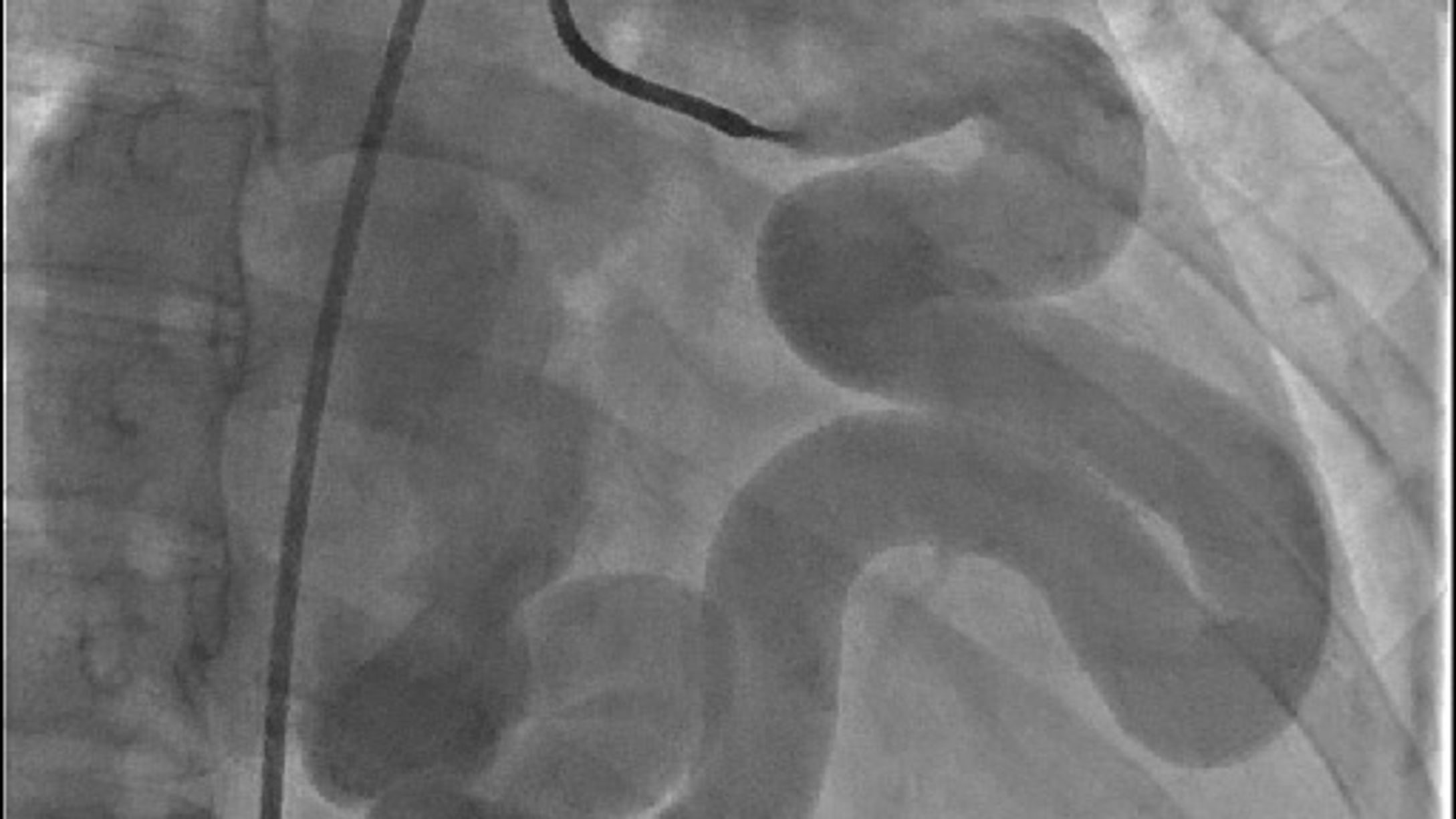
1
Diagnostic angiogram
Distal coronary branch in myocardium
Expert Approaches
Hover over an experts image to view their approach.
Dr. Ryan Callahan
MD, FSCAI
Boston Children's Hospital
Division of Invasive Cardiology
Assistant Professor of Pediatrics, Harvard Medical School
-
Patient is symptomatic with highQp:Qs. Aim for partial closure to reduce Qp:Qs and prevent proximal pathologic remodeling.
-
“Whisper” 0.014’’ super floppy wire with hydrophilic tip to pass fromLCA to atrium.
-
Snare wire in RA and establish AV loop.
-
Advance catheter of choice into distal fistula (hydrophilic Bentson)and deploy a couple coils.
-
Home on coumadin/ASA and consider recath in 6 months
Dr. Matt Crystal
MD, FACC, FSCAI
New York-Presbyterian & Morgan Stanley Children's Hospital
Assistant Professor of Pediatrics, Columbia University Medical Centre
Associate Director, Pediatric Cardiac Catheterization Cardiology
-
Answer: Would you close... and approach andtherapy post•I would recommend closure given the patient symptoms, significantleft-to-right shunt and size of the fistula. Access distal to the coronaryartery branches should be obtained and then consideration for eithercomplete occlusion or partial occlusion to try to avoid significantthrombosis of the dilated “conduit” proximal coronary. If distal accessis obtained can consider closure withamplatzerdevices or theMedtronic MVP 9Q. Post-occlusionheparinizationas a bridge untiltherapeutic on Coumadin. Dual therapy with aspirin to be considered and then single therapy with aspirin after 6-12 months of coumadin and confirmatory cath/angiography to document absence of thrombi and/or assess potential for remodelling
Dr. Harsimran SIngh
MD, MSc
Director, Adult Congenital Heart Disease,
Director, Cardiovascular Disease Fellowship, Weill Cornell Medicine
-
Yes, I would close. Would give ASA and heparin on table while doing this case. Would try to close distally
-
Anterograde bring balloon further down to clarify outlet of fistula and size
-
Externalize a coronary wire into the right side – snare to create an arteriovenous rail.
-
From venous side bring sheath – given size this may be suitable for AVP-4 at distal outlet.
-
ASA and coumadin (bridged after the case) – observe on telemetry unit for 24 hours
Dr. Allison Calbalka
MD, FSCAI
Professor of Pediatrics, Mayo Clinic College of Medicine
Consultant, Pediatric Cardiology
Director, Congenital Cardiac Laboratory
Mayo Clinic, Rochester, Minnesota
-
She is symptomatic and likely to become more so over time. CTA for pre-procedure mapping.
-
Retrograde coronary guide with Glide cath and/or microcatheter to advance 0.035” exchange length angled Glidewire through fistula past RA entry point; snare via SVC or Femoral and create a rail. Measure fistula diameter at largest point.
-
Bring 8-10 Fr shuttle sheath into RA fistula entry point over rail, deploy large AVPII in distal fistula (2-4 mm >> fistula diameter); one disc past entry
-
Consider deploying larger packable/detachable coils from aortic end distal in fistula near plug, extend proximal but NOT proximal to the NORMAL coronary branches-watch ECG
-
Long-term anticoagulation with warfarin and ASA (risk of thrombosis with large prox. CA, but if some residual flow might have less chance of clot!)
Dr. Zahid Amin
MD, FSCAI, FAHA, FAAP
William B. Strong Chair and Professor and Section Chief
Division of Pediatric Cardiology
Congenital and Structural Heart Disease
Children’s Hospital of Georgia, Augusta University
-
Close it. I would use KA micro plug since it can go through 3F and we can use co-axial system to put the plugs. I would not mind if there is residual shunt that may close over extended period of time.